- On February 10, 2025
Employer-sponsored health plans that offer prescription drug coverage to Medicare-eligible individuals must meet an important annual reporting requirement: submitting the Disclosure to CMS Form to confirm whether their prescription drug coverage is creditable or non-creditable compared to Medicare Part D.
With the deadline approaching, plan sponsors should ensure they file their disclosure on time to avoid compliance issues. Below is an overview of the reporting requirements and key deadlines.
Who Needs to File the Disclosure?
Employer-sponsored health plans must submit the Disclosure to CMS Form if they offer prescription drug benefits to any Medicare-eligible individuals, including:
- Active employees
- Retirees
- COBRA beneficiaries
- Disabled individuals
- Dependents of Medicare beneficiaries
What is the Purpose of the Disclosure?
The disclosure informs the Centers for Medicare & Medicaid Services (CMS) whether the employer’s prescription drug coverage is creditable (expected to pay at least as much as Medicare Part D) or non-creditable (not expected to meet this standard).
This determination is essential because:
- Medicare beneficiaries need this information to decide whether to enroll in Part D. If their employer coverage is non-creditable, they may face late enrollment penalties if they delay signing up for Medicare Part D.
- Employers that fail to file the disclosure on time risk compliance issues and potential penalties.
When is the CMS Disclosure Due?
The Disclosure to CMS Form must be submitted within 60 days after the start of the plan year for employer-sponsored health plans that offer prescription drug coverage. Additionally, employers must file within 30 days if they terminate prescription drug coverage or change its creditable status.
CMS Disclosure by Plan Year
Below is a breakdown of the disclosure deadlines based on the plan’s start date:
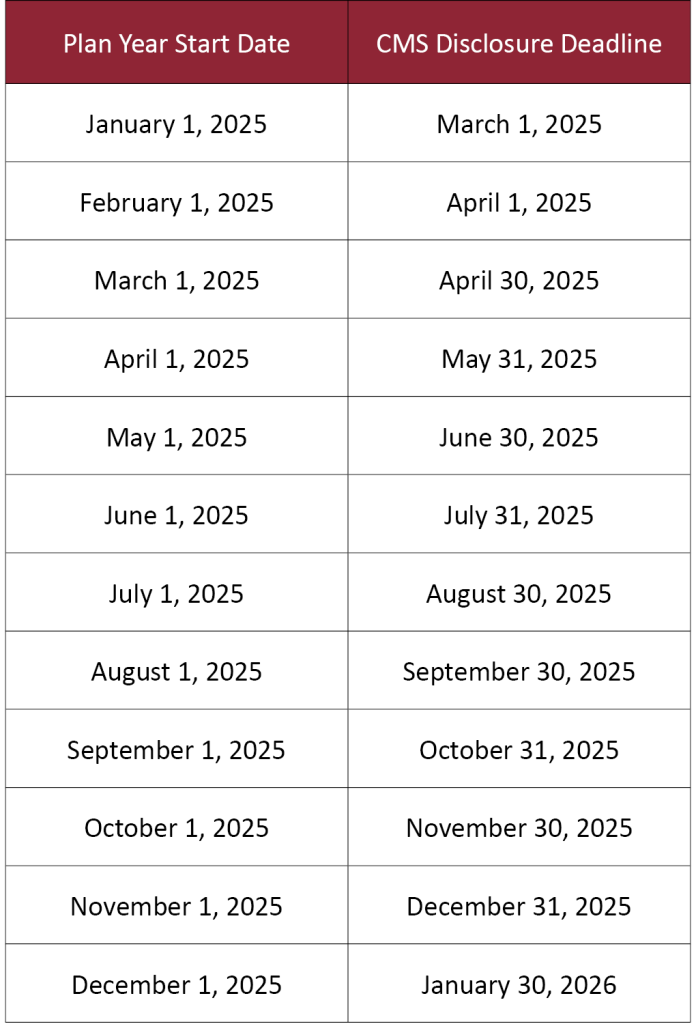
Employers should verify their plan year start date and ensure they meet the corresponding deadline.
How to Submit the Disclosure to CMS
Employers must complete and submit the Disclosure to CMS Form electronically through the CMS website at CMS Creditable Coverage Disclosure. The process is straightforward and typically takes less than 15 minutes.
Final Reminders
- Employers should review their Creditable Coverage Notices sent to Medicare-eligible individuals by October 15 each year.
- The CMS disclosure must be completed separately and is due within 60 days of the plan year start date.
- Employers should retain documentation of their submissions for compliance purposes.
As the deadline approaches, plan sponsors should act promptly to ensure compliance and avoid potential issues for Medicare-eligible individuals covered under their plans.
